The Centers for Medicare and Medicaid Services released 2007 US healthcare spending data in late December. Since then several publications have come out analyzing this information. The most comprehensive is probably a Health Affairs article which highlighted a slowdown in the growth in spending for prescription drugs and government administration.
The Center for American Progress also recently issued a paper comparing the US healthcare system in 2007 to the situation in 1994. This paper concluded:
“The status quo of American health care is spending more money to cover fewer people, yielding disappointing outcomes. Effective reforms, which would invest in measures to improve the quality and delivery of care, reform payment to reward outcomes, and provide affordable, accessible, comprehensive health insurance for all Americans, are long overdue. The best time to fix American health care was over a decade ago. The second best time is now.”
While it is certainly true that the US healthcare system has evolved greatly since 1994, not everything has gone in the wrong direction. There have certainly been improvements in therapies and data collection and analysis tools – primarily through computerized information technologies. And while, it is certainly true that our healthcare system isn’t producing the clinical outcomes that are widely believed possible, the good news is that the rate of spending increases appears to be slowing – see chart below.
US National Health Spending Annual Increases: Actual and CPI Adjusted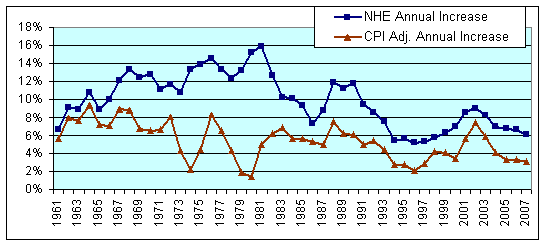
Sources: CMS & BLS
Causes of Changing Rates in Increased Health Spending
Closer examination of the healthcare spending trends reveals that there have been peaks and valleys. The increasing rates leading up to the peak in 2001 is believed to be due to the declining influence of managed care in the mid to late 1990s, when employers were striving to hire and keep workers in the booming economy. Since finding and retaining employees was so hard, containing healthcare costs became secondary to making employees happy. Of course, after the economy stumbled in 2000, not surprisingly, the growth in healthcare spending also declined.
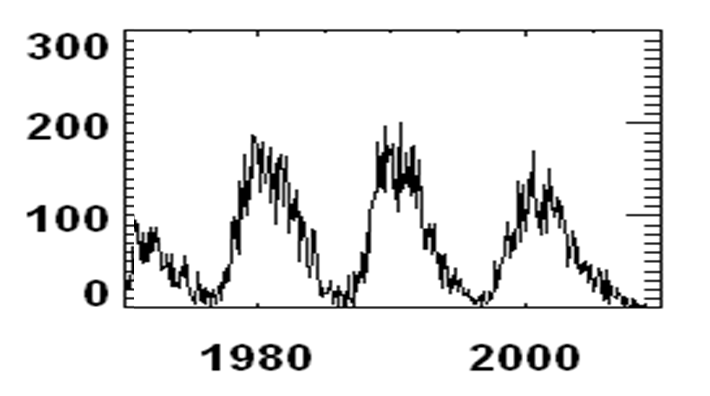
An alternative explanation for the timing of the peaks and valleys in the rate in healthcare spending could also be the number of sunspots. As can be seen in the chart below, (see peaks in 1979, 1990 and 2001), there is a correlation between the 11 yearly cycle of peaks in sunspot activity and the rates of increase in healthcare spending. [This “clearly” demonstrates that correlation probably doesn’t not prove causation – since it could also be posited that greater rates of increasing health spending in the United States “causes” sunspot.]
Back to the Reality of Increasing Healthcare Spending
From the first chart it can be seen that the rate of increasing health spending has declined each year since 2002. Looking forward, it appears that the economic downturn in the second half of 2008 is reigning in healthcare spending. Therefore, it would not be surprising if the trend in the growth in health spending continues to decline into 2009, and the CPI adjusted growth rate heads toward zero.
However, additional health spending in the Federal stimulus legislation and/or in health reform could bump up health spending. While increased spending in certain areas of heatlhcare can certainly be worthwhile investments, the rhetoric of healthcare policy seems to always present a contradictory proposition, i.e. more healthcare spending to create jobs and improve the economy is good, but at the same time increasing spending more than GDP growth is bad…… This conundrum seems like trying to have your cake and eat it too.
Next Steps in Health Reform
What is missing or minimized in most of the discussions about increasing health spending is how the the structure and operations of the healthcare delivery system is a fundamental factor causing and maintaining high health spending. Health reform proposals often avoid directly addressing changing the organization of healthcare delivery because it is a complicated, daunting task, and physicians, other clinicians and their patients present a very strong, locally effective lobbying force.
However effective organizations such at the Institute for Healthcare Improvement have made great strides in the care delivered in hospitals, and the Medicare Payment Advisory Committee and physician organizations have made recommendations involving concepts such as Medical Homes, which involve transforming clinical care delivery – although there may be differences in what each organization means by “Medical Homes” and similar terms, and how the proposed changes would actually increase integration and accountability.
Connection Between Transforming Outpatient Clinical Care and Healthcare Spending
The connection between outpatient care and health spending is illustrated in the pie chart (see below) of where US healthcare spending goes:
US Health Spending in 2007 By Type of Service and Activity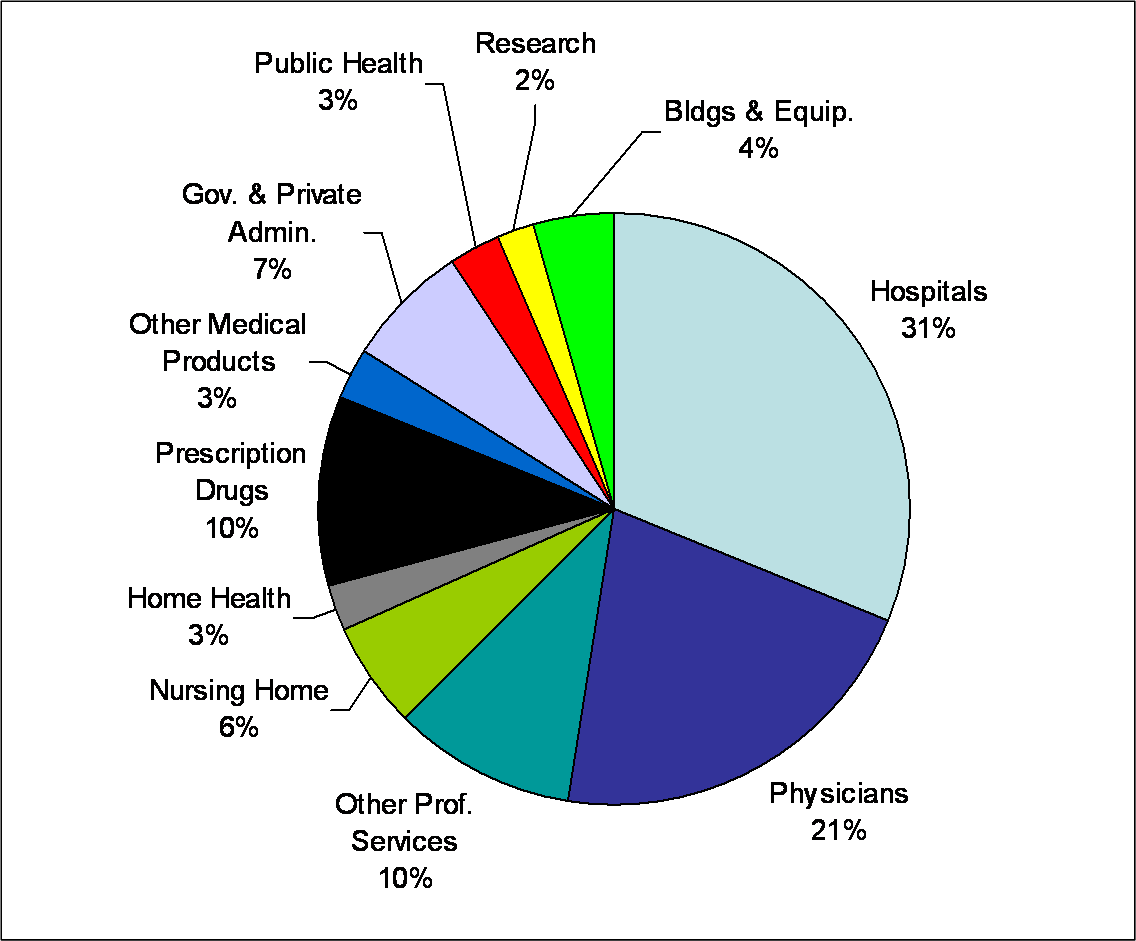
Source: CMS
As can be seen, while physicians receive 21% of all health spending in the US, their actions control another 50-60% – so they directly or indirectly are responsible for 70-80% of the $2.2 Trillion in health spending. Therefore, it should be obvious that it will be crucial to change how healthcare is delivered if health care costs are to be controlled. And just as obvious is that reforming healthcare delivery will require physicians’ involvement and support. Otherwise, even the best planned and intentioned efforts will fall short of controlling costs and improving quality.
(p.s. Last summer I wrote about the the trends in this health spending and the confusion some physicians have about these numbers. This post might also be of interest.)

[…] I thought it would be useful to update the pie chart I’d posted previously that showed 2007 and 2006 National Health Expenditures. So below is the chart showing US health spending for […]
Pat – Thanks for your comment. There have been many analyses of healthcare administrative costs. The numbers I used are the National Health Expenditure data collected by CMS – which is one of the fundamental data sources for healthcare spending in the US. Other analyses I’m aware of have tried to look at isolated pieces of administrative costs – and most have poor methodology. The one area of increased administrative costs where there seems to be some agreement is that premiums paid by individuals and very small employers are higher because managing contracts to such small numbers has higher per enrollee costs than what is seen for large groups. (Of course this is not unique to health insurance – selling anything wholesale or in large multi-unit packages – as seen at COSTCO – has lower per unit transaction costs than selling something retail or one at at time.) This reality is one of the reasons supporting the creation of health insurance exchange, such as we have here in MA. However, as the Texas example showed, exchanges need to be carefully constructed so that there is not adverse selection to purchase through the exchange – this will lead to the typical (and predictable) cost spiral leading to the demise of the exchange. The Massachusetts Connector – which is an exchange – was constructed with this in mind, so it has not suffered that fate.
I understand that health insurance companies incur as much as 30% overhead costs and that doctors often spend many hours per week in overhead arguing with health insurers. These costs are considerable: as much as $400B per year. Can you include those costs explicitly in an analysis?
Thanks.
[…] Power of the Pen I also described for the physicians at Carney Hospital how as information systems become more sophisticated and can provide insights into the performance of smaller groups and individual physicians, more proposals and initiatives will seek to place greater accountability on the individual physicians because while physicians receive ~21% of all healthcare spending in this country, their actions influence ho… […]
[…] that physicians direct most clinical decisions and thus influencing overall healthcare spending, it is not surprising that third party programs were ineffective in changing clinical or cost […]
There was a time when, if you wanted to become a physician, the bankrolling required more than the velleity of simply making the making the choice and the financing appears.
Then in the 1950’s and 1960’s the (then) HEW came up with what seemed a simple solution to the health care conundrum: financial aid to medical schools. They planned to flood the market with new MD’s and so cause increased competition to lower the cost factor attributable to doctors’ incomes.
In the mid 1970’s I was a dinner guest of a brilliant couple of Washington health apparatchiks. He was (among other things) guiding the nascent EPSDT program. And she (the sister of one of the Brookings Institution’s leading economists) was eventually to become the Director of the National Center for Health Statistics. In short, not only were they broadly wired into the beltway health establishment, they had their hands on the steering wheel.
Another guest that evening was the wife of a health economist who had recently been jilted by her co-researcher husband. And she was getting back at him by blabbing about the results of their latest findings, before they had been published: financial support of medical education was having the opposite effect on health costs than they had anticipated!
Although the money given to Medical Schools had worked to increase the supply of physicians, there hadn’t been the expected depressive influence on doc’s incomes. They had found that wherever there were new MD graduates, they would produce medical care and make a handsome income while doing it. The equation was more docs=more procedures and higher medical costs—not lower fees.
By producing more Docs, Washington had increased the supply of costly medical care providers who continued to command a great return on the investment the government had made in their education.
There was amused consternation around the dinner table. Medical Economics had not responded to the “Law” of supply and demand. “Well, maybe we’ll do better with this new entity, The HMO.”
A Need To Reformulate
The following are facts that are believed to exist regarding the present U.S. Health Care System. This may be why about 80 percent of U.S. citizens understandably want our health care system overhauled:
The U.S. is ranked number 42 related to life expectancy and infant mortality, which is rather low.
However, the U.S. is ranked number one in the world for spending the most for health care- as well as being number one for those with chronic diseases. About 125 million people have such diseases. This is about 70 percent of the Medicare budget that is spent treating these terrible illnesses. Health Care costs are now well over 2 trillion dollars of our gross domestic product. This is three times the amount nearly 20 years ago- and 8 times the amount it was about 30 years ago. Most is spent with medical institutions, as far as health expenditures are concerned. One third of that amount is nothing more than administrative toxic waste that does not involve the restoration of the health of others. This illustrates how absurd the U.S. Health Care System is presently. Nearly 7000 dollars is spent on every citizen for health care every year, and that, too, is more than anyone else in the world.
We have around 50 million citizens without any health insurance, which may cause about 20 thousand deaths per year. This includes millions of children without health care, which is added to the planned or implemented cuts in the government SCHIP program for children, which alone covers about 7 million kids.
Our children.
Nearly half of the states in the U.S. are planning on or have made cuts to Medicaid, which covers about 60 million people, and those on Medicaid are in need of this coverage is largely due to unemployment. With these Medicaid cuts, over a million people will lose their health care coverage and benefits to a damaging degree.
About 70 percent of citizens have some form of health insurance, and the premiums for their insurance have increased nearly 90 percent in the past 8 years. About 45 percent of health care is provided by our government- which is predicted to experience a severe financial crisis in the near future with some government health care programs, it has been reported. Most doctors want a single payer health care system, which would save about 400 billion dollars a year- about 20 percent less than what we are paying now. The American College of Physicians, second in size only to the American Medical Association, supports a single payer health care system. The AMA, historically opposed to a single payer health care system, has close to half of its members in favor of this system. Less than a third of all physicians are members of the AMA, according to others.
Our health care we offer citizens is the present system is sort of a hybrid of a national and private health care system that has obviously mutated to a degree that is incapable of being fully functional due to perhaps copious amounts and levels of individual and legal entities.
Health Care must be the priority immediately by the new administration and congress. Challenges include the 700 billion dollars that have been pledged with the financial bailout that will occur, since the proposed health care plan of the next administration is projected to cost over a trillion dollars within the first year or so of the proposed plan to recalibrate health care for all of us in the U.S. Yet considering the hundreds of billions of dollars that are speculated to be saved with a reform of the country’s health care system, health policy analysts should not be greatly concerned on the steakholders who may be affected by this reform of our health care system that is desperately needed. Tom Daschle leads this Transition’s Health Policy Team. And we also have Ed Kennedy, the committee chair and a prolific legislator. So if the right people have been selected for this reforming team, the urgency and priority regarding our nation’s health care needs should be rather overt to the country’s citizens.
Half of all patients do not receive proper treatment to restore their health, it has been stated. Medical errors desperately need to be reduced as well, it has been reported, which should be addressed as well.
It is estimated that the U.S. needs presently tens of thousands more primary care physicians to fully satisfy the necessities of those members of the public health. This specialty makes nearly 100 thousand less in income compared with other physician specialties, yet they are and have been the backbone of the U.S. health care system. PCPs manage the chronically ill patients, who would benefit the most from the much needed coordination and continuity of care that PCPs historically have strived to provide for them. Nearly have of the population has at least one chronic illness- with many of those having more than one of these types of illnesses. A good portion of these very ill patients have numerous illnesses that are chronic, and this is responsible for well over 50 percent of the entire Medicare budget.
The shortage of primary care physicians is due to numerous variables, such as administrative hassles that are quite vexing for these doctors, along with ever increasing patient loads complicated by the progressively increasing cost to provide care for their patients. Many PCPs are retiring early, and most medical school graduates do not strive to become this specialty for obvious reasons. In fact, the number entering family practice residencies has decreased by half over the past decade or so. PCPs also have extensive student loans from their training to complicate their rather excessive workloads as caregivers.
Yet if primary care physicians were increased in number with the populations they serve and are dedicated to their welfare. Studies have shown that mortality rates would decrease due to increased patient outcomes if this increase were to occur. This specialty would also optimize preventative care more for their patients. Studies have also shown that, if enough PCPs are practicing in a given geographical area, hospital admissions are decreased, as well as visits to emergency rooms. This is due to the ideal continuity in health care these PCPs provide if they are numbered correctly to treat and restore others. Also, the quality improves, as well as the outcomes for their patients. Most importantly, the quality of life for their patients is much improved if there are enough PCPs to handle the overwhelming load of responsibility they presently have due to this shortage of their specialty that is suppose to increase in the years to come. The American College of Physicians believes that a patient centered national health care workforce policy is needed to address these issues that would ideally restructure the payment policies that exist presently with primary care physicians.
Further vexing is that it is quite apparent that we have some greedy health care corporations that take advantage of our health care system. Over a billion dollars was recovered for Medicare and Medicaid fraud last year through settlements paid to the department of Justice because some organizations who deliberately ripped off taxpayers. These are the taxpayers in the U.S. who have a fragmented health care system with substantial components and different levels of government- composed of several legal entities and individuals, which has resulted in medical anarchy, so it seems.
Health 2.0, a new healthcare social networking innovation, is informing patients about their symptoms and potential if not possessing various disease states- largely based on the testimonies of other people on various websites. This may be an example of how so many others rely now on health concerns from those who likely are not medical specialists, instead of becoming a participant, if not victim, of the U.S. Health Care System.
Thanks to various corporations infecting our Health Care System in the United States, the following variables sum up this system as it exists today, which is why the United States National Health Insurance Act (H.R. 676) is the best solution to meet our health care needs as citizens, it appears. We would finally have, as with most other countries, a Universal Health Care system that will allow free choice of doctors and hospitals, potentially. It should be and likely will be funded by a combination of payroll taxes and general tax revenue:
Access- citizens do not have the right or ability to make use of this system as we should.
Efficiency- this system strives on creating much waste and expense as it possibly can.
Quality- the standard of excellence we deserve as citizens with our health care is missing in action.
Sustainability- We as citizens cannot continue to keep our health care system in as it is designed at this time- as it exists today.
http://www.mckinsey.com/mgi/publications/US_healthcare/index.asp
Dan Abshear