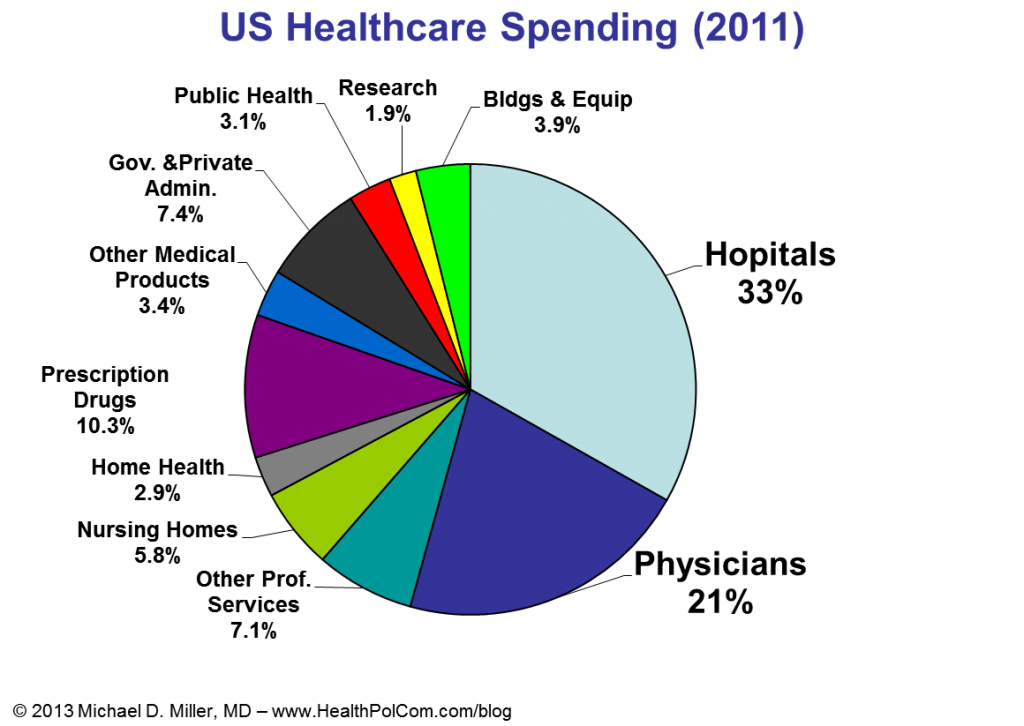
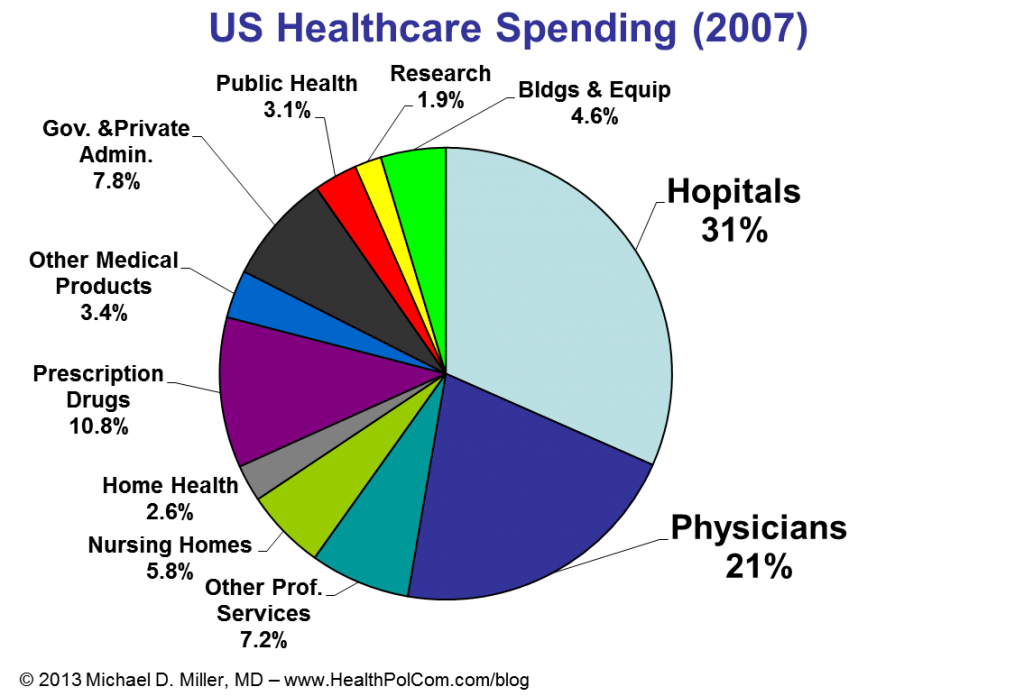
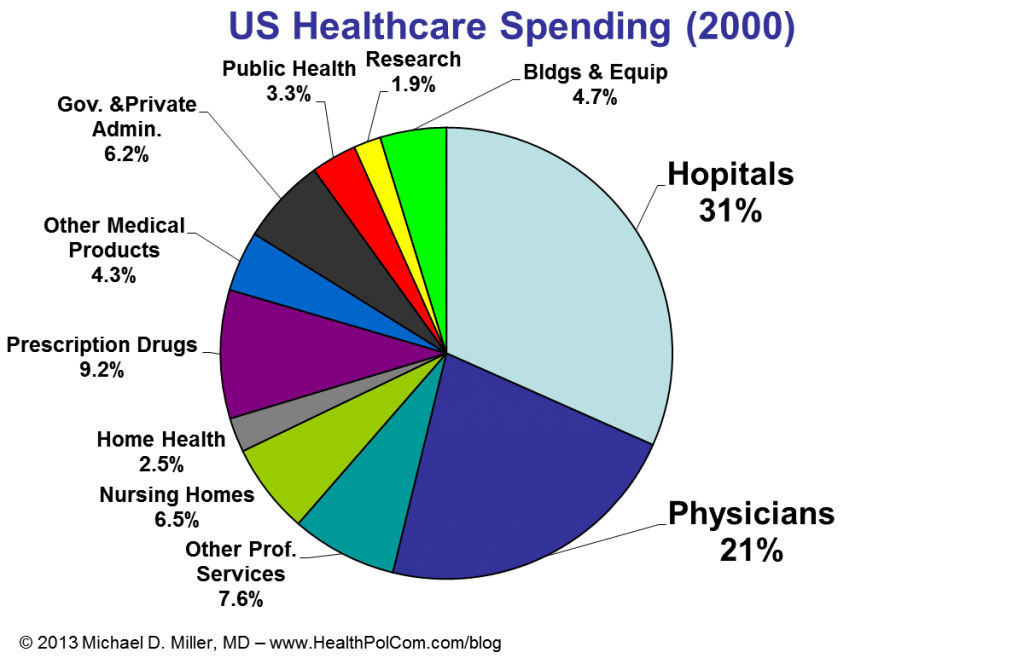
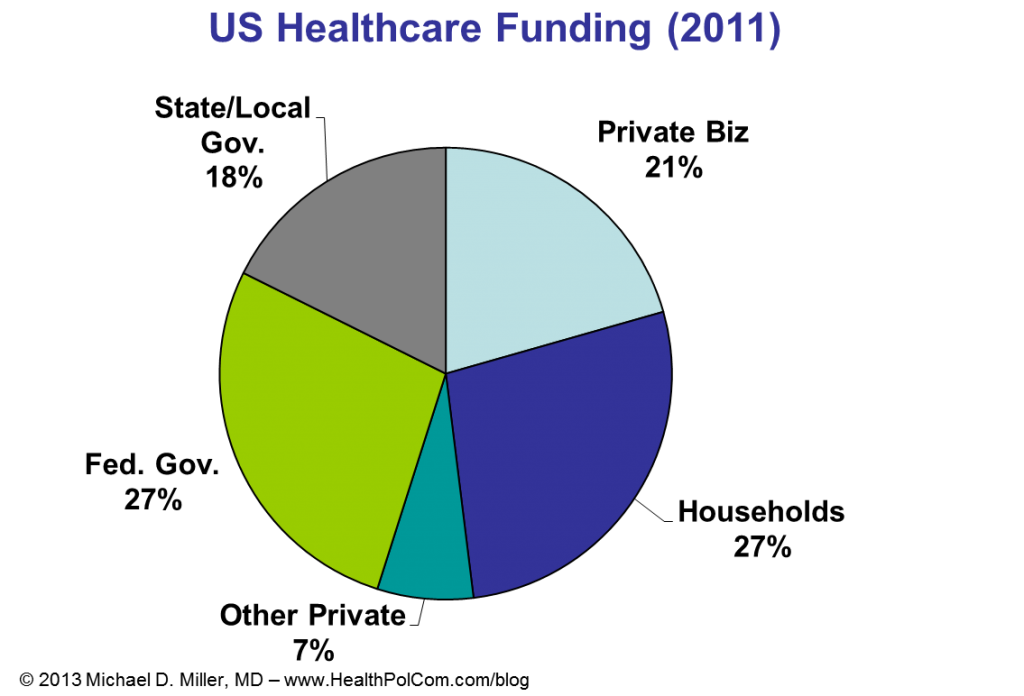
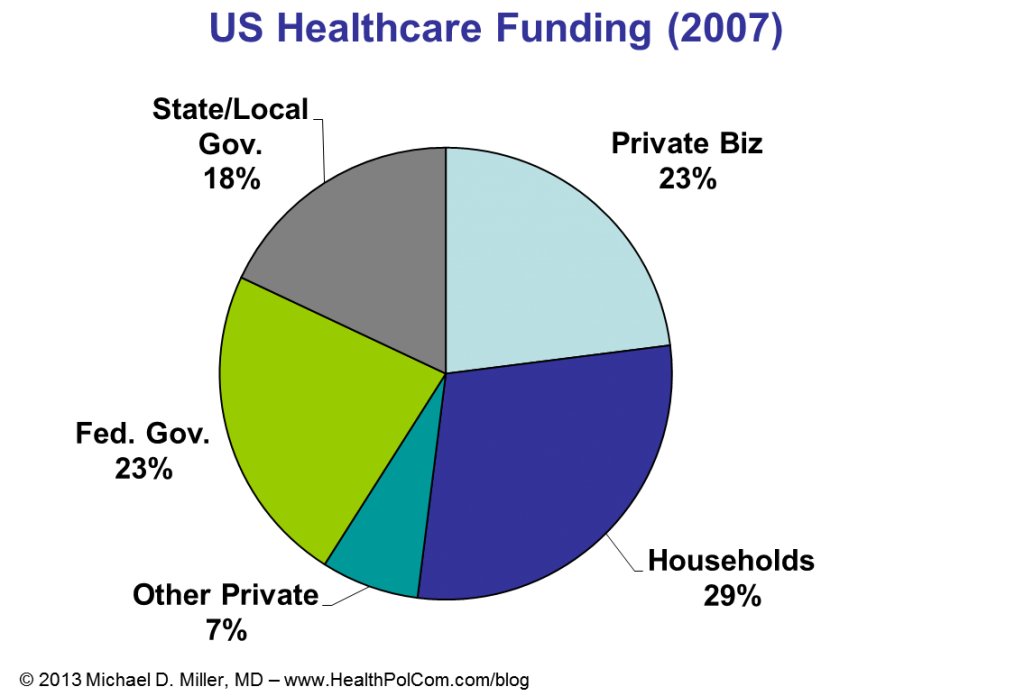
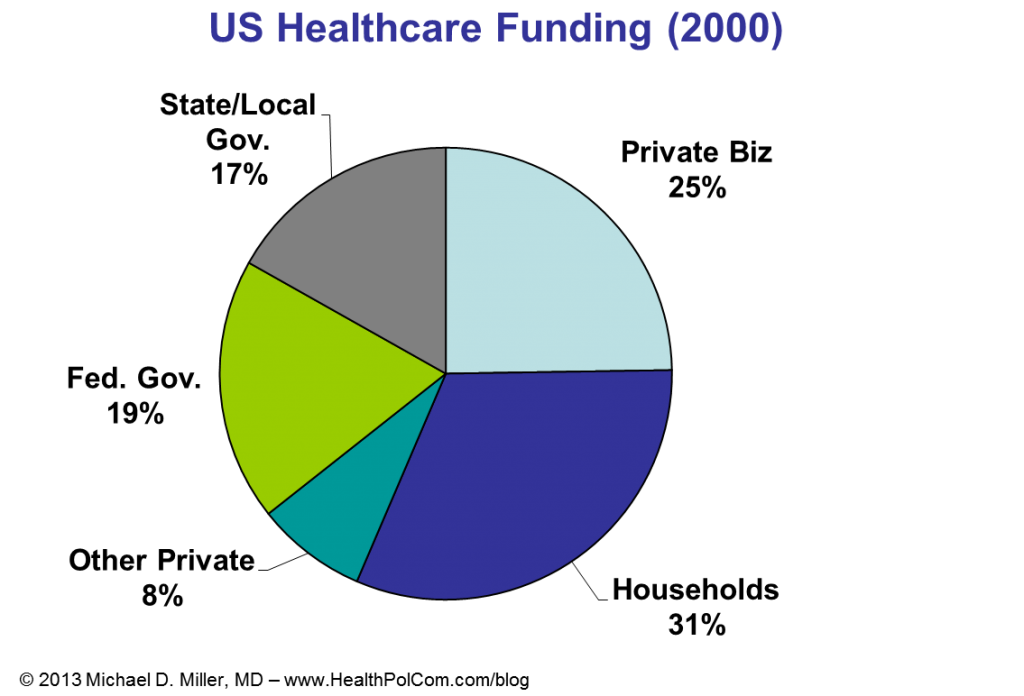
I recently had the opportunity to give guest lectures at Georgetown University and the University of Virginia. At Georgetown I focused on employer’s perspectives on health promotion and disease prevention. (Videos of portions of that discussion are below.) At UVA’s Batten School of Public Policy I discussed fiscal issues and policies for government healthcare programs, e.g. Medicare and Medicaid. (A few slides from that discussion are below….. sorry no video.)
The opportunity to talk with our future clinicians, health system administrators, and policy makers was heartening and a bit terrifying. While the students are eager and passionate, I wonder about their historical understanding of our complex healthcare systems and the policies, programs, and initiatives that got us to where we are today.…